Bias in Facial Recognition Technology
Tania Firouzbady. 07/10/2021
![]()
Antibiotic resistance has become a pivotal topic for biomedical research in recent years. Its ability to hinder advancements in drug development makes it one of the biggest threats to public health. Each year, approximately 2.8 million people in the United States develop an infection due to antibiotic resistance.
In simple terms, antibiotics are chemicals that inhibit the growth of microorganisms such as bacteria and fungi. They accomplish this by either directly killing the microorganism or by stopping its reproduction long enough for the host’s immune system to kick in. To better understand the various components of the immune system, it’s important to first discuss the human microbiome.
The human microbiome refers to the sum of all the microorganisms, or microbes, living in the human body. These microbes include eukaryotes, bacteria, archaea, and viruses. Research indicates that there are about ten times as many microbial cells as there are human cells. While it may seem surprising that microbes are such an important part of the body–after all, antibiotics are meant to target them–it is important to note that not all microbes are the same; some are harmful while others are beneficial.
The microbiome is closely linked to the immune system. According to the journal Cell Research, “The microbiome plays critical roles in the training and development of major components of the host’s innate and adaptive immune system, while the immune system orchestrates the maintenance of key features of host-microbe symbiosis.” In other words, the microbiome and immune system have a mutually beneficial relationship because they rely on each other to operate.
The immune system is responsible for getting rid of pathogens, or disease-causing microbes. White blood cells are one of the most important parts of the immune system. Certain types of white blood cells, namely B and T lymphocytes, are memory cells, meaning they remember a pathogen after its first invasion and produce antibodies, proteins that protect against pathogens, much more quickly in subsequent infections. These cells are part of the acquired immune system, which changes throughout an organism’s life.
Different from the adaptive immune system, the acquired immune system is inherited at birth and remains unchanged over time. During a pathogenic infection, the innate immune system sends phagocytes, a type of cell that can engulf bacteria and particles, to attack the invading cells. Through these mechanisms, both the innate and acquired immune systems work together to ward off pathogens.
Antibiotics often work in conjunction with the immune system to prevent the spread of pathogens. One well-known antibiotic is penicillin, which is used to treat staphylococci and streptococci bacterial infections. The former is a skin infection that typically results from an open wound or surgery, while the latter is a mouth/throat infection. Penicillin works by damaging bacterial cell walls.
A vital aspect of such antibiotic development is ensuring that they don’t harm people. Since humans lack cell walls, they are unaffected by penicillin treatment. According to News Medical, “Penicillin kills bacteria through binding of the beta-lactam ring to DD-transpeptidase, inhibiting its cross-linking activity and preventing new cell wall formation.” To put it simply, by binding to an enzyme (DD-transpeptidase), penicillin forms a highly stable intermediate that prevents the enzyme from functioning, which ultimately inhibits cell wall formation.
Antibiotic resistance is caused by genetic mutations in bacteria, which are more prone to mutations due to their rapid rate of reproduction. When bacteria reproduce in the vicinity of antibiotics, already present mutations that allow them to be resistant are passed onto future generations, eventually leading to the evolution of a resistant strain. Hence, the antibiotic becomes ineffective, and a stronger one is needed. Over time, as this cycle continues and antibiotics become stronger, their production will become impractical. Even more worrisome is the fact that “bacterial strains can become resistant to more than one antibiotic, leading to the creation of ‘superbugs’ that are extremely difficult to treat.”
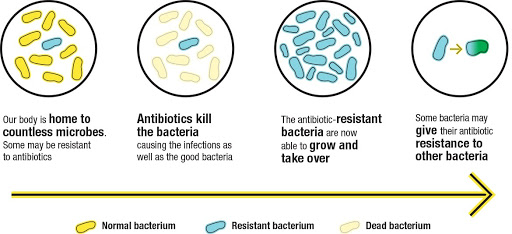
Bacteria achieve resistance to antibiotics through various mechanisms. Penicillin resistance, for example, was the direct result of bacterial production of beta-lactamase, an enzyme that harms the beta-lactam ring. Without it, penicillin is no longer capable of damaging bacterial cells.
As time goes on, antibiotic resistance and the creation of superbugs has become more widespread. Fortunately, awareness of the issue has also increased and scientists are developing new methods to combat antibiotic resistance. One such method is focusing attention on natural antibiotics rather than artificial ones.
Scientists from the Institute for Stem Cell Science and Regenerative Medicine have been doing just this. As outlined by phys.org, “the team probed the cellular mechanisms that regulate the release of antimicrobial peptides (AMPs), which are natural antibiotics produced by skin cells to fight off bacteria.” What makes AMPs unique is that they attack bacteria in ways that make resistance to them very difficult. By understanding the mechanisms used by AMPs, researchers may be able to develop antibiotics that replicate them. Moreover, the research has already led to a groundbreaking discovery: skin cells utilize a signaling pathway that regulates how AMPs are released, meaning that by altering these pathways, scientists can allow the AMPs to be released without being exposed to the bacteria at all. This could potentially help groups of people that are in greater danger of infection, including those with a weak immune system.
Cover Photo: (The Conversation)
